Diabetes and Kidney Health: A Toolkit for Clinicians
April 18, 2021 · Matt Brock
Let’s Talk About Diabetes and Kidney Health.
Diabetes is prevalent in 10% of U.S. adults (34 million people) and is a leading cause of chronic kidney disease (CKD). African American, Hispanic and American Indian patients are disproportionately at high risk for kidney disease, in part due to higher rates of diabetes in these communities.
Even though chronic kidney disease leads to progressive loss of kidney function, people suffering from the condition often don’t feel symptoms until the late stages of the disease. Nine of every 10 adults with CKD are unaware they have it. And it has repercussions beyond kidneys. CKD increases the risks of heart disease, stroke and early death, in addition to kidney failure. Early diagnosis and treatment can prevent or at least slow chronic kidney disease. That’s why ongoing monitoring of kidney health is crucial for people with diabetes.
Clinical practice guidelines from the American Diabetes Association and the National Kidney Foundation (NKF) recommend screening patients with diabetes for kidney disease every year using estimated Glomerular Filtration Rate (eGFR) and urine Albumin-to-Creatinine Ratio (uACR).
Two Tests Assess Kidney Health
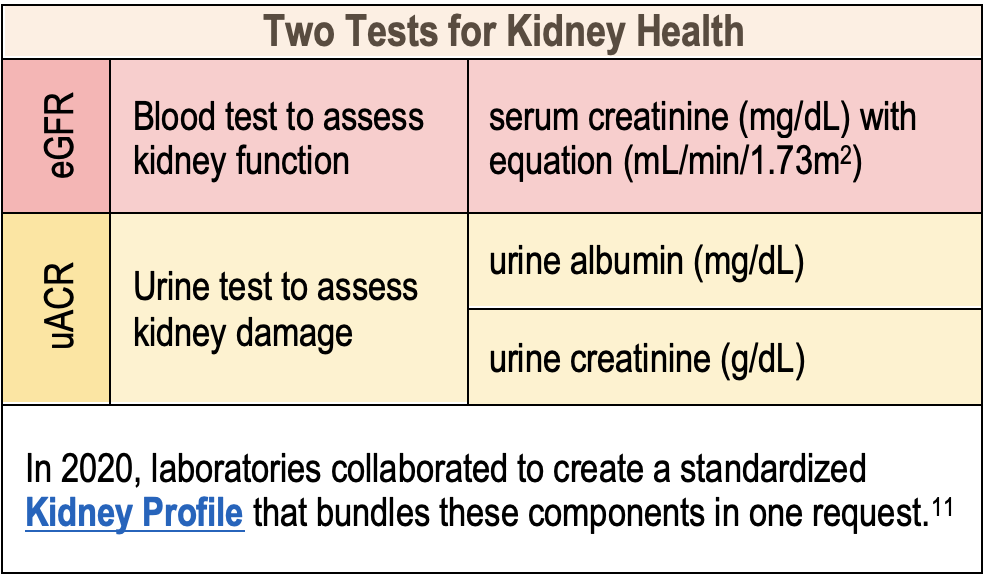
Kidney damage is assessed using uACR based on a spot urine sample, recommended by guidelines because it is unaffected by variation in urine concentration. Other tests for albumin, such as a dipstick, are not recommended because they are less
sensitive and do not detect lower uACR levels.
Kidney function is assessed using eGFR based on the patient’s serum creatinine level, age, sex and race, but clinicians are currently reevaluating the use of race in calculating kidney function. The NKF-ASN (American Society of Nephrology) Task Force on Reassessing the Use of Race in Diagnosing Kidney Disease is working toward a national solution to eGFR reporting (a final report is expected in 2021). ,
Together, these two tests provide key information regarding kidney health, including determining the stage of CKD and the risk of progression. So, laboratories collaborated to create a standardized Kidney Profile that bundles these components in one request. Elevated uACR is often the earliest sign of CKD. Rising uACR (≥30 mg/day) detection occurs about 10 years before a detectable decline in eGFR and thus is an early indicator of kidney disease in patients with diabetes.
Two Tests, One Lab Request, One Performance Measure
Evidence shows that contrary to clinical guidance, fewer than half of people with diabetes receive an annual kidney assessment that includes both eGFR and uACR. Kidney Health Evaluation for Patients With Diabetes (KED) addresses this gap. KED is a new HEDIS® measure in its first year of implementation, with public reporting of results expected in 2022. The Centers for Medicare & Medicaid Services will report KED on its display page for 2022 Star Ratings and will consider adding it to Star Ratings in the future.
Test results are used to diagnose and code a patients’ CKD stage and are often secondary to a code for the underlying cause, such as diabetes or hypertension. Test results can also be used to educate patients about kidney disease and the elevated risk for those with diabetes. Educational resources to support conversations, including videos addressing the risk of kidney disease and handouts explaining kidney test results, are available from the National Institute of Diabetes and Digestive and Kidney Diseases.
So, regular monitoring of kidney health is clearly an identified priority.
The Resource
Primary care practices specifically play a key role in treating kidney disease through managing risk factors such as hypertension or hyperglycemia, prescribing medications and encouraging a healthy lifestyle. Primary care clinicians also play a pivotal role in determining when to refer to a specialist. So, NCQA, with the financial support of Bayer Healthcare Pharmaceutical, Inc.B, has composed a toolkit to help you navigate and sustain this new recommended approach. It includes a heat map that will help you analyze test results and provide benchmarks for additional tests or a referral to a nephrologist.
But the key is to start with regular testing, and then to use results to better advise and educate your patients.








