Movements in Medicaid: Tennessee Ties Quality to Payments
January 12, 2018 · Amy Maciejowski
Many states work diligently to improve the quality of health care, and we want our programs to help guide their mission. Specifically, states can leverage NCQA’s Health Plan Accreditation to drive quality improvement for its Medicaid population.
Tennessee Medicaid (TennCare) continues to be ahead of the curve! The state was first in the nation to implement a comprehensive managed care model for Medicaid, way back in 1994. Tennessee has successfully intertwined its and NCQA’s goals of cutting costs and improving quality and outcomes. Here’s how:
Tennessee Required Health Plan Accreditation. TennCare requires all Medicaid Managed Care Organizations (MCOs) to be NCQA Accredited. State officials note that requiring TennCare plans to be NCQA Accredited “made it easier for the state to implement an incentive program tied to HEDIS measures.”
Tennessee Tied Quality Improvement to Payments Using NCQA’s HEDIS Measures. TennCare instituted a pay-for-performance incentive program for MCOs. As part of the accreditation journey, organizations report their performance on Healthcare Effectiveness and Data Information Set (HEDIS®) measures. TennCare used HEDIS data to focus on quality improvement.
Because children make up a large portion of TennCare members, Tennessee selected a handful of HEDIS measures related to children’s preventive services. MCOs were expected to improve performance on these measures in order to be eligible for an incentive payment.
Tennessee Monitored Improvement. According to a National Academy for State Health Policy case study “as of 2015, 85% of the 33 HEDIS measures tracked since 2007 have shown improvement over time, and 47 measures improved from 2014 to 2015.”
Tennessee’s in Good Company
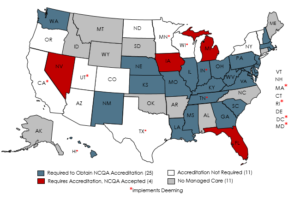
This is just one example of using innovative methods to improve care delivery. Currently, twenty-five Medicaid Managed Care states require NCQA Health Plan Accreditation as part of contracting requirements. An additional four states require accreditation and accept NCQA Health Plan Accreditation.
For more information on NCQA’s work with states, click here.








