CPC+ Announces Regions – View NCQA directory as a tool!
August 1, 2016 · Amy Maciejowski
On August 1, CMS announced the states and regions selected to participate in the new Comprehensive Primary Care Plus (CPC+) program. CPC Plus offers a unique opportunity to gain additional assistance for sustaining your primary care practice transformation. Practices accepted into CPC+ get per-member-per-month payments ranging from $15 up to $100. Under proposed rules for the Medicare Access and CHIP Reauthorization Act, they would also be Advanced Alternative Payment Models that get automatic 5% bonuses on all Medicare Part B billing. The deadline to apply for CPC+ is September 15. NCQA supports CPC Plus, which offers an opportunity for practices to get additional financial resources while reducing burden by aligning with other payers.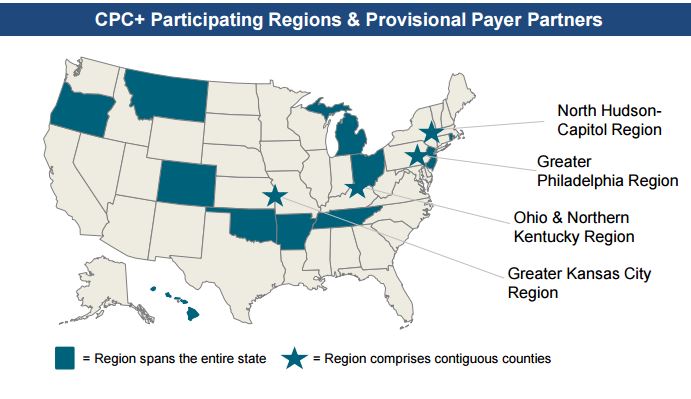
Directory of Initiatives Supporting NCQA Clinical Programs
To coincide with the CPC Plus announcement, NCQA recently released a directory that links clinicians to local resources (financial and other) that support NCQA clinical Recognition programs. However, financial incentives listed in the directory may not be available for all providers in the network. We encourage you to check with the appropriate payer representative.
The directory includes a list of public, private and multi-payer initiatives, by state, that support a variety of NCQA clinical Recognition programs:
- Patient Centered Medical Home (PCMH).
- Patient Centered Specialty Practice (PCSP).
- Patient Centered Connected Care.
- Diabetes Recognition Program (DRP).
- Heart/Stroke Recognition Program (HSRP).
Why Use The Directory?
The directory can be a tool for all states and regions, whether or not they participate in CPC Plus
State/Region Selected to Participate in CPC Plus
Your practice should apply—this is an opportunity to see financial rewards (especially from Medicare) for a commitment to primary care transformation. We encourage you to connect with other payers in your state or region because they might offer additional incentives or support, building on your investment and increasing the likelihood of sustained transformation. Refer to the directory for a list of organizations and initiatives providing support in your state or region.
State/Region Not Selected to Participate in CPC Plus
There are many resources available to support your investment in primary care transformation. Refer to the directory for a list of organizations and initiatives providing support in your state or region.
As Medicare prepares to support PCMHs more broadly with automatic credit in the new Merit-Based Incentive Payment System (MIPS), which adjusts clinician payment based on performance, there is a greater case for transforming into a PCMH. MIPS takes effect in 2019, but payment adjustments will be based on 2017 performance. Rules are not yet final, but are likely to reward clinicians for being in NCQA-Recognized PCMHs during 2017.








